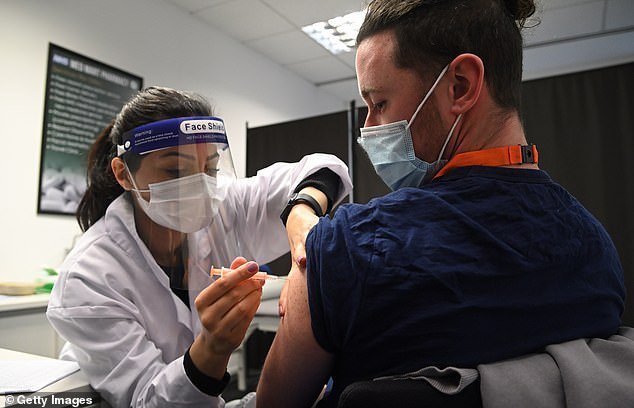
Spacing Oxford University’s Covid vaccine doses 12 weeks apart actually boosts the jab’s effectiveness, according to a study which suggests the UK’s dosing gamble has paid off.
When the second injection is given after three months the vaccine prevents 81 per cent of people from getting symptomatic illness.
But when there is only between three and six weeks between the doses its efficacy is just 55 per cent, according to Oxford’s own analysis, published in The Lancet.
With many vaccines, the longer the gap between doses can lead to better results – the HPV vaccine for girls, for example, works better when given after a year as opposed to a month. It’s thought that a longer time period ‘primes’ the immune system, giving it time to process and store genetic instructions on how to defend against the virus.
Crucially for Britain’s current strategy, the first dose offers 75 per cent protection on its own for 12 weeks. Immunity kicks in after 22 days following vaccination.
But the researchers are urging people to have two doses of the vaccine because they say it is not yet clear how long protection with a single dose of the vaccine may last.
A study in Israel on the Pfizer vaccine found it was 85 per cent effective after the first dose, adding more support to Britain’s decision to delay the second injection.
The UK drew criticism in January when it pushed back giving second doses of both vaccines from three weeks to three months because the jabs were never trialled using that dosing regimen.
The policy recommendation was made by the Joint Committee on Vaccination and Immunisation (JCVI) as the country grappled with the highly virulent Kent variant and limited vaccine supplies. Its goal was to get wider coverage more quickly.
Spacing Oxford University’s Covid vaccine doses 12 weeks apart actually boosts the jab’s effectiveness, a study has found


Study lead author Professor Andrew Pollard, University of Oxford, said: ‘Vaccine supply is likely to be limited, at least in the short term, and so policy-makers must decide how best to deliver doses to achieve the greatest public health benefit.
‘Where there is a limited supply, policies of initially vaccinating more people with a single dose may provide greater immediate population protection than vaccinating half the number of people with two doses.
‘In the long term, a second dose should ensure long-lived immunity, and so we encourage everyone who has had their first vaccine to ensure they receive both doses.’
Researchers combined data from trials in the UK, Brazil, and South Africa, including 8,948, 6,753, and 1,477 people, respectively – totalling 17,178 people.
Participants were aged 18 years and over and either received two standard doses of the Oxford vaccine (8,597 participants) or a placebo.
Looking at the interval between two standard doses and its impact on efficacy, participants who were given their doses 12 or more weeks apart had greater protection (81 per cent) than people given their two doses less than six weeks apart (55%).
The results were supported by immune response results in 18-55-year-olds, which found that binding antibody responses were more than two-fold higher in the group having their two vaccines with a longer delay.
Following a single standard vaccine dose, vaccine efficacy from 22 days to three months after vaccination was 76%, researchers found.
Modelling indicated that this protection did not reduce over the three months.
In addition, antibody levels against the coronavirus spike protein remained at similar levels for three months, according to the study.
The authors estimate that a single dose of the vaccine may lead to a 64 per cent reduction in community transmission, and that two doses may reduce cases by 50 per cent.
The effect of two doses appears less than a single dose because there are more asymptomatic cases included in this part of the analysis, and vaccine efficacy against asymptomatic cases is lower.
Professor Pollard said real-world assessments of how the vaccine is working in the population will be needed to confirm this preliminary result.
It comes after an Israeli study published today found Pfizer/BioNTech’s coronavirus vaccine is 85 per cent effective after the first dose.
The research on 9,000 healthcare workers, published in The Lancet, found that a single shot reduced the number of people developing symptomatic Covid by 85 per cent after three weeks.
Separate research by Pfizer/BioNTech published today showed their vaccine can now be stored at the same temperature as a household freezer (-15C to -25C) for two weeks rather than at the ultra-cold -70C. This could dramatically expand the rollout of the jabs, and rule out the logistical nightmare of moving doses in specialist containers keeping them at ultra-low temperatures.
The company has submitted its results to the US-based Food and Drug Administration (FDA) to approve the change to shipping requirements, reports the Financial Times, with experts saying it’s likely the pharmaceutical giant has now had enough time to test the jab at different temperatures.
The study on the effectiveness of the jabs after one dose was carried out by the Sheba Medical Centre, one of Israel’s top research hospitals. It reported a 75 per cent drop in the number of people testing positive for the infection, suggesting the single shot will have a significant impact on blocking asymptomatic infection and transmission.
A positive PCR swab would signal that even someone who is vaccinated is carrying fragments of the virus in their nose or throat which they could pass on. Reducing Covid’s spread is critical for country’s to achieve ‘herd immunity’, when so many people are immune that a disease peters out.
Lead researcher Professor Arnon Afek, deputy director-general at Sheba, said: ‘This groundbreaking research supports the British government’s decision to begin inoculating its citizens with a single dose of the vaccine.’